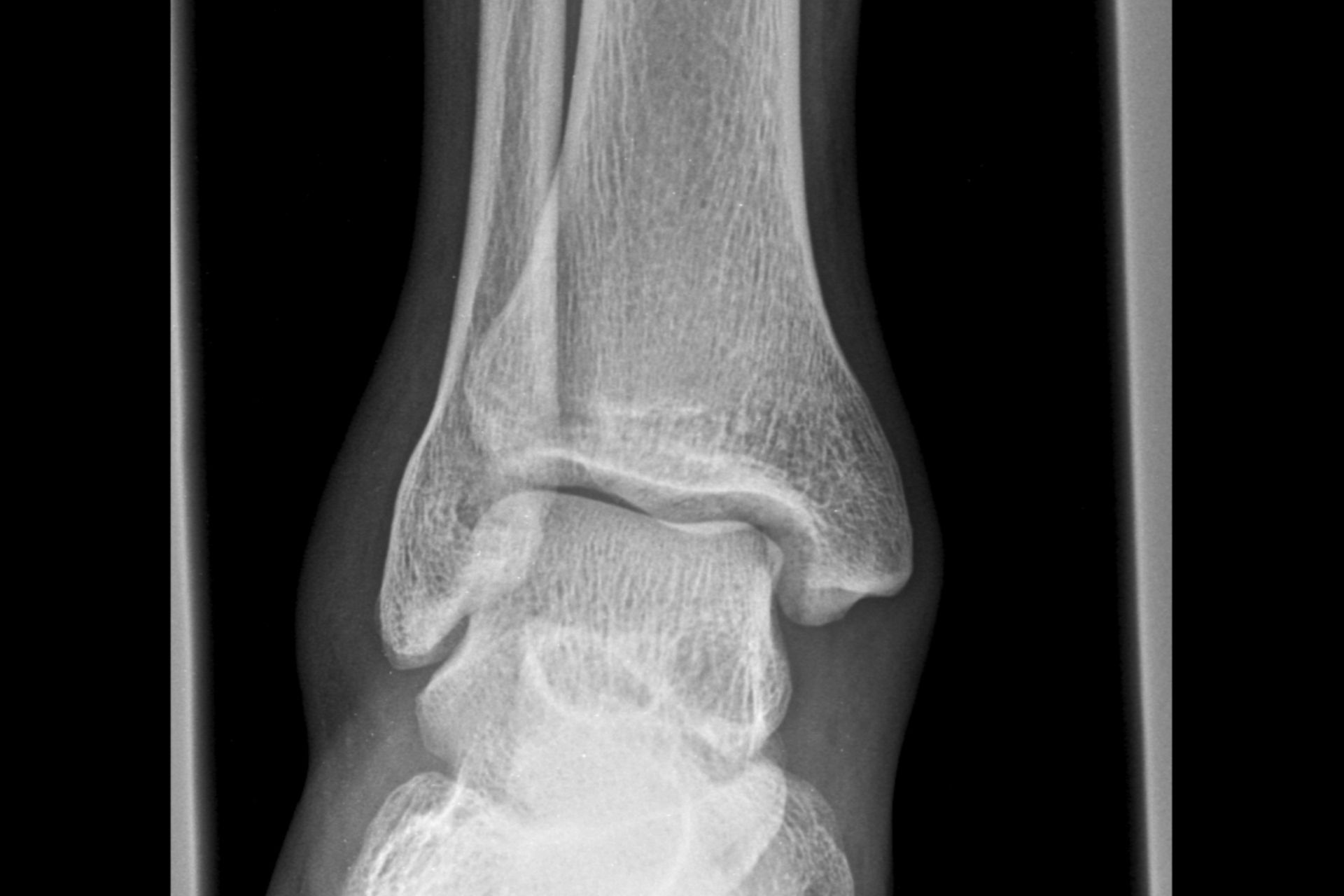
Your feet contain dozens of joints that work together to absorb shock, support balance, and propel you forward with every step. Because they carry your full body weight, these joints experience constant stress throughout your life. Osteoarthritis is a degenerative joint condition that gradually wears down protective cartilage, leading to friction, inflammation, and structural changes. While many people associate it with knees or hips, the feet are frequently affected. Understanding how this condition progresses in the feet helps you recognize early signs and take steps to protect mobility and comfort as you age.
Understanding Osteoarthritis in Foot Joints
Osteoarthritis develops when the cartilage that cushions joints begins to thin and break down. Cartilage normally allows bones to glide smoothly against each other. When it deteriorates, bones experience increased friction. This triggers inflammation, swelling, and pain. The foot has many small joints, especially in the midfoot and toes, making it vulnerable to wear over time. Repetitive pressure, prior injuries, genetic factors, and alignment issues can accelerate the process. Unlike a sudden injury, this condition progresses gradually. Many people do not realize what is happening until stiffness and discomfort begin interfering with daily activities.
Early Changes You Might Notice
The earliest signs often appear subtly. You may feel stiffness in the morning that improves with movement. Shoes that once felt comfortable may begin to feel tight or irritating. Mild aching after long walks or standing can become more frequent. Some people notice a reduced range of motion in their toes or midfoot joints. These early signals are easy to dismiss as normal aging or fatigue, but they indicate that cartilage is beginning to lose resilience. Paying attention at this stage allows for early management strategies that slow progression and reduce long-term damage.
Progression of Joint Stiffness
As osteoarthritis advances, stiffness becomes more persistent. Joints that once loosen after a few steps may remain tight throughout the day. This stiffness changes how you walk. The body naturally tries to avoid painful motion, leading to altered gait patterns. When movement becomes restricted, surrounding muscles compensate, which can create fatigue and imbalance. Over time, limited flexibility in the feet affects posture and strain travels upward to the ankles, knees, and hips. Many people do not connect these secondary pains to their foot joints, but the chain reaction begins at the base.
Pain and Inflammation Over Time
Pain from osteoarthritis is not always constant in early stages, but it tends to increase as cartilage continues to wear down. The joint lining becomes inflamed, producing swelling and tenderness. Activities that place pressure on the feet, such as walking long distances or standing on hard surfaces, may trigger flare-ups. Some people experience sharp pain during movement, while others feel a dull ache that lingers after activity. In advanced stages, discomfort may appear even at rest. Chronic inflammation can also lead to warmth and visible swelling around affected joints.
Structural Changes in the Feet
Long-term joint degeneration can alter foot structure. As cartilage thins and bones respond to increased stress, the body may form small bony growths known as bone spurs. These growths attempt to stabilize the joint but often restrict movement further. Toes may begin to drift or overlap, and the arch may change shape depending on which joints are affected. These structural shifts influence weight distribution, creating new pressure points that can lead to calluses and irritation. The longer the condition progresses without support, the more pronounced these changes may become.
Impact on Balance and Mobility
Healthy feet provide a stable platform for balance. When joints become painful or stiff, that stability decreases. People with advanced osteoarthritis may walk more cautiously to avoid discomfort. This cautious movement can reduce stride length and slow walking speed. Balance may feel less secure, increasing the risk of falls. Everyday activities such as climbing stairs, standing from a seated position, or carrying groceries can become more challenging. Mobility loss affects independence and quality of life, which is why early intervention is so important.
Secondary Effects on Other Joints
The body works as an interconnected system. When the feet change how they absorb force, the rest of the body adapts. Altered walking patterns place extra stress on the ankles, knees, hips, and lower back. Over time, these areas may develop their own discomfort or inflammation. Some people treat knee or back pain without realizing the original source lies in their feet. Addressing joint health at the base of the body often reduces strain higher up the chain. Proper support and treatment can restore more natural movement patterns.
Emotional and Lifestyle Impact
Chronic foot pain affects more than physical movement. It influences mood, activity levels, and social engagement. People may avoid exercise or outings that require walking, which can lead to reduced fitness and isolation. Fear of pain sometimes causes individuals to become sedentary, which further weakens muscles and joint support. Maintaining activity is essential for joint health, so managing symptoms effectively has both physical and emotional benefits. Understanding the condition helps people make informed choices rather than withdrawing from movement altogether.
Managing Osteoarthritis in the Feet
While osteoarthritis cannot be reversed, its impact can be managed. Supportive footwear plays a critical role. Shoes with cushioning, proper arch support, and a wide toe box reduce pressure on irritated joints. Custom orthotics can redistribute weight more evenly, relieving stress on damaged areas. Gentle stretching and strengthening exercises improve joint flexibility and muscle support. Low-impact activities such as swimming or cycling maintain mobility without excessive strain. Weight management also reduces pressure on foot joints, slowing further wear.
The Importance of Professional Care
Professional evaluation helps tailor treatment to your specific joint pattern. A foot specialist can assess alignment, joint mobility, and pressure distribution. Treatment may include orthotic support, targeted therapy, and strategies to control inflammation. Early care prevents small limitations from becoming severe disability. Regular monitoring allows adjustments as the condition evolves. Many people experience significant relief once their movement patterns are supported properly. Ignoring symptoms allows degeneration to progress unchecked, making management more difficult later.
Protecting Long-Term Foot Function
Long-term joint health depends on proactive care. Listening to your body, wearing appropriate footwear, and staying active within comfortable limits all contribute to preserving mobility. Small adjustments made early have lasting benefits. Protecting your feet protects your independence. The goal is not to stop movement but to move smarter. With proper support, many people continue active lifestyles despite joint changes.
If you are experiencing foot pain or stiffness related to osteoarthritis, schedule a visit with Steady Foot Clinic in North York for expert assessment and personalized care.